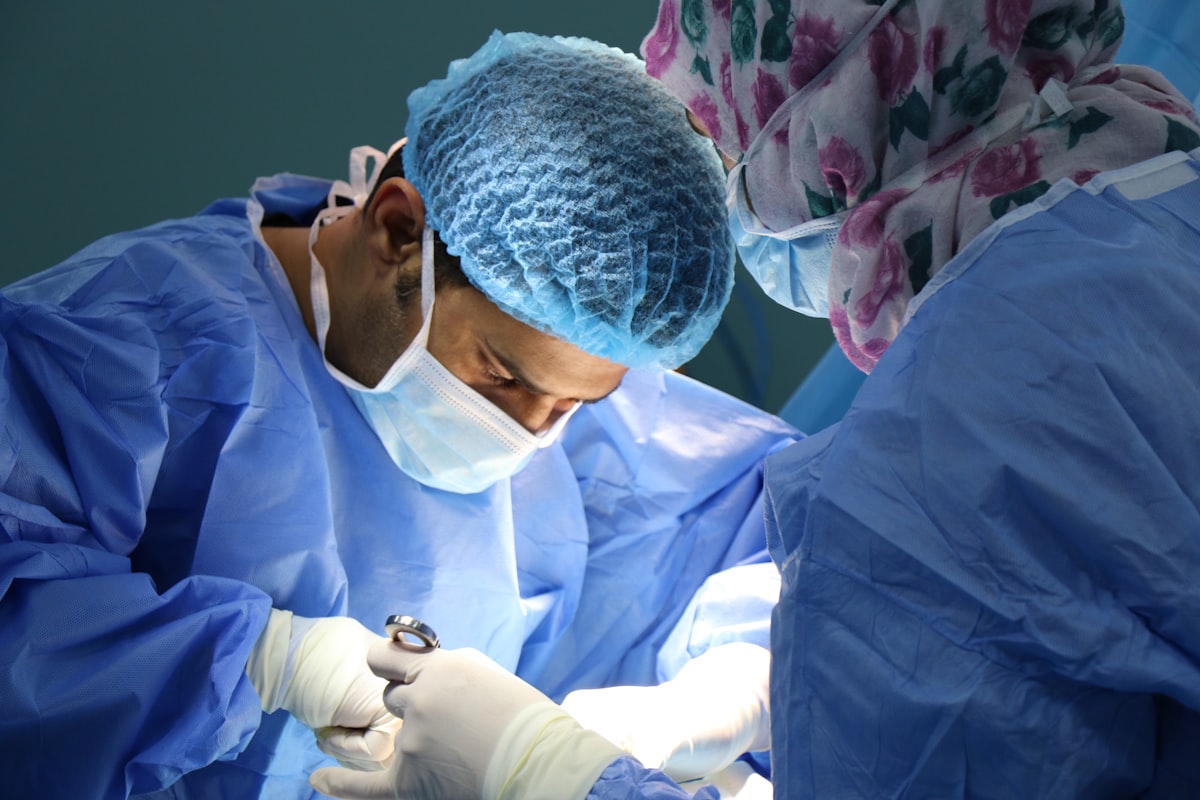
Every year, millions of workers are injured on the job. The path back to work — navigating medical assessments, employer accommodations, insurance adjudication, and rehabilitation — is one of the most administratively intensive processes in the healthcare system. It is also one of the most consequential. Research consistently shows that the longer a worker is away from employment, the harder the return becomes — psychologically, physically, and financially.
AI-powered occupational health software is changing this equation. By automating the intake, triage, documentation, and case coordination tasks that consume occupational health professionals' time, artificial intelligence is enabling faster assessments, more consistent outcomes, and better experiences for injured workers. This is not a future trend — it is happening now, across insurers, employers, and occupational health clinics worldwide.
This article explores where automation is making the greatest impact in return-to-work (RTW) programs, what the technology actually does, and what occupational health organisations need to consider before implementing it.
Key Takeaways
- Delayed return-to-work has measurable negative outcomes for workers — speed and consistency of assessment directly improves results.
- AI automates the most time-consuming administrative tasks in RTW case management, freeing clinicians for higher-value work.
- Natural language processing can extract structured clinical data from unstructured physician reports, dramatically accelerating adjudication.
- Predictive analytics can identify workers at risk of prolonged absence before it happens, enabling early intervention.
- AI-assisted functional capacity tools are increasing objectivity and reducing variability in return-to-work assessments.
- Implementation must account for privacy regulation, clinician trust, and the need for human oversight in clinical decisions.
The Return-to-Work Challenge

Return-to-work programs sit at the intersection of healthcare, employment law, insurance, and workplace safety. A single case may involve a treating physician, an occupational health nurse, a case manager, an employer HR representative, a workers' compensation adjuster, a physiotherapist, and a vocational rehabilitation specialist — all exchanging information through a combination of fax, email, phone calls, and disconnected software systems.
The administrative overhead is enormous. Studies have found that case managers in disability and occupational health settings spend more than 40% of their time on documentation, coordination, and communication tasks that add no direct clinical value. Meanwhile, claims that sit in administrative queues waiting for a missing report or an unanswered phone call are exactly the claims that end in prolonged absence, litigation, and poor outcomes for everyone involved.
The Cost of Delay
The occupational health research is unambiguous: early intervention and rapid RTW assessment produce better outcomes than delayed, thorough ones. Workers who return to modified duties within two weeks of injury have significantly better long-term functional outcomes than those who remain off work for two months — even when the clinical presentation is identical at the time of injury.
This means that speed is not a trade-off against quality in return-to-work assessment. Speed, when achieved through better process and better tools rather than clinical shortcuts, is itself a clinical quality measure. AI's primary contribution to occupational health is making fast, consistent, well-documented assessment achievable at scale.
Automated Intake and Triage

The first point of friction in most RTW programs is intake — the process of receiving an injury report, gathering the necessary information, assigning it to the right case manager, and ensuring that no critical step is missed in the first 24–48 hours. Done manually, this process is error-prone, time-consuming, and heavily dependent on individual staff knowledge.
AI-powered intake systems replace static forms with dynamic, adaptive questionnaires that respond to the answers provided. If a worker reports a back injury, the system automatically prompts for relevant clinical detail — mechanism of injury, radiation, neurological symptoms — that would be absent from a generic intake form. If the employer is in a high-risk industry, additional safety and compliance questions are added automatically.
This dynamic intake approach ensures that the information needed for triage is collected at first contact, eliminating the most common cause of early case delays: incomplete intake documentation requiring follow-up calls.
Automated Triage and Case Assignment
Once intake is complete, AI triage engines analyse the submitted information against predictive models to assign a complexity score and urgency flag to each case. Cases flagged as high complexity — those involving mental health comorbidities, prior claims history, disputed liability, or specific injury types associated with prolonged absence — are routed immediately to senior case managers. Routine cases follow automated workflows that reduce the need for manual coordination.
This ensures that clinical expertise is directed where it makes the greatest difference, while administrative capacity handles the high volume of straightforward cases that currently consume the same resources as complex ones.
Natural Language Processing for Clinical Documentation

One of the most transformative applications of AI in occupational health is natural language processing (NLP) applied to clinical documentation. Physician reports, specialist letters, and treatment notes are almost universally written in unstructured free text. Extracting actionable information from them — functional limitations, diagnosis codes, treatment recommendations, expected recovery timelines — currently requires a trained human to read every document.
Structuring Unstructured Reports
NLP models trained on occupational health documentation can extract structured clinical data from physician reports automatically. A report that arrives as a scanned PDF or a plain-text email can be processed by an NLP engine that identifies:
- Primary diagnosis and relevant ICD codes
- Specific functional limitations (lifting restrictions, sitting tolerance, driving restrictions)
- Expected return-to-work date and any stated conditions
- Recommended treatment modalities and referrals
- Flag phrases indicating psychological factors, disputed causation, or legal representation
This extracted data is then automatically populated into the case management system, triggering the appropriate next steps — employer notification, modified duties assessment, or specialist referral — without requiring a case manager to read and re-enter the information manually.
Consistency Across Cases
Beyond efficiency, NLP brings consistency to a process that is highly variable when done manually. Two case managers reading the same physician report may extract different information, apply different interpretations, and make different adjudication decisions. NLP applies a consistent extraction model across every document, every time — reducing variability and improving the auditability of decisions.
Predictive Analytics and Early Intervention
Perhaps the most clinically significant application of AI in return-to-work is predictive modelling — using case data to identify workers at elevated risk of prolonged absence before the prolonged absence happens. This enables the early intervention that the occupational health evidence base consistently shows produces the best outcomes.
Predicting Prolonged Absence
Predictive return-to-work models are trained on historical claims data to identify the combination of clinical, demographic, workplace, and psychosocial factors that are associated with delayed recovery. These models can assess new cases on day one and flag those likely to require intensive case management — allowing resources to be deployed proactively rather than reactively.
Key predictive factors that AI models identify include:
- Prior claims history and prior episodes of absence
- Injury type and mechanism
- Industry and job demands relative to functional limitations
- Presence of comorbid mental health conditions
- Workplace relationship quality indicators (e.g., reports of supervisor conflict)
- Time elapsed between injury and first clinical contact
- Treatment adherence signals in early case activity
Enabling Proactive Case Management
When a case is flagged as high-risk on day two, a case manager can contact the worker before a pattern of disengagement sets in. They can coordinate a multidisciplinary team, arrange early physiotherapy, facilitate a modified duties conversation with the employer, and address psychosocial barriers before they become entrenched. This proactive model produces measurably better outcomes than reactive case management — and AI-powered risk stratification makes it operationally feasible at scale.
AI-Assisted Functional Capacity Evaluation

A Functional Capacity Evaluation (FCE) is a structured assessment of a worker's physical ability to perform job-specific tasks. It is a cornerstone of the return-to-work decision — providing objective evidence of what a worker can and cannot safely do. Traditionally, FCEs are conducted in person by an occupational therapist or physiotherapist over several hours, and the results are documented in a narrative report.
Variability and Objectivity Challenges
The challenge with traditional FCEs is variability. Results can differ based on the assessor's experience, the effort level of the worker being assessed, the time of day, and subtle differences in test administration. This variability undermines the credibility of FCE results in contested claims and creates inconsistency in modified duties recommendations across cases with similar clinical presentations.
Technology-Augmented Assessment
AI-assisted assessment tools are addressing this variability in several ways:
- Wearable sensor integration — accelerometers and force sensors that capture objective biomechanical data during functional tasks, independent of assessor interpretation
- Effort validity algorithms — AI models that analyse performance patterns to identify submaximal effort, reducing the impact of poor effort on assessment validity
- Structured digital protocols — guided assessment applications that ensure consistent test administration regardless of assessor experience level
- Automated report generation — AI systems that translate assessment data directly into structured reports, reducing documentation time and improving standardisation
These tools do not replace the clinical judgment of the occupational therapist — they augment it with objective data and consistent documentation, making assessments more defensible and more consistent across a large caseload.
Automated Case Coordination and Communication

Beyond the clinical components of return-to-work, a substantial amount of case management time is spent on coordination and communication — notifying employers of restrictions, following up on outstanding medical reports, scheduling appointments, and updating insurance adjusters. AI-powered workflow automation handles these tasks systematically.
Automated Employer Communication
When a physician report arrives and functional limitations are extracted by the NLP system, an automated workflow can immediately notify the employer's HR representative with a structured summary of the worker's restrictions and a modified duties request. The employer receives actionable information within minutes of the report being processed, rather than waiting for a case manager to find time to make a call.
Intelligent Follow-Up and Escalation
AI-driven case management systems monitor case activity and trigger automated follow-up actions when expected milestones are not met. If a specialist referral was made but no appointment confirmation has been received within three business days, the system automatically escalates to the case manager. If a worker has not attended a scheduled physiotherapy appointment, an alert is generated before the absence becomes a pattern.
This intelligent monitoring ensures that cases do not stall in administrative queues without anyone noticing — one of the most common causes of poor outcomes in traditional case management.
Considerations for Implementation

The benefits of AI in occupational health are real, but implementation requires careful planning. Organisations that rush deployment without addressing the following considerations often find that adoption fails regardless of the quality of the technology.
Privacy and Data Governance
Occupational health data is among the most sensitive personal data in existence. It contains medical histories, mental health information, injury details, and employment records. Any AI system that processes this data must comply with applicable privacy legislation — HIPAA in the United States, PIPEDA in Canada, GDPR in Europe — and must implement data minimisation, access controls, audit logging, and retention policies appropriate to regulated health information.
Before deployment, document your data flows. Understand where worker data goes, who can access it, and how long it is retained. Your workers and their representatives will ask these questions, and the answers must be clear.
Clinician Trust and Change Management
AI tools in occupational health will only deliver value if the clinicians and case managers who use them trust the outputs. A predictive model that flags cases as high-risk must be explainable — the case manager needs to understand why a case was flagged, not just that it was. Systems that produce recommendations without explanation create resistance rather than adoption.
Invest in training and change management. Involve clinicians in the selection and configuration of tools. Treat AI as a decision support system that augments clinical expertise, not one that replaces it.
Human Oversight in Clinical Decisions
Regulatory and ethical standards require that consequential clinical decisions — return-to-work clearance, functional capacity conclusions, treatment recommendations — remain under human oversight. AI should automate the information gathering, documentation, and administrative coordination that surrounds these decisions. The clinical judgment must remain with a qualified professional.
Design your workflows accordingly. AI handles the preparation; humans own the decisions.
FAQ
Can AI replace an occupational health nurse or case manager?
No — and that is not the right goal. AI automates the administrative, documentation, and coordination tasks that currently consume 40–50% of an occupational health professional's time, freeing them to focus on the clinical, relational, and complex judgment tasks that AI cannot perform. The result is a case manager who can handle a larger, more complex caseload more effectively — not a case manager replaced by software.
How accurate are AI-based predictive RTW models?
The most mature predictive models in workers' compensation and disability management settings achieve AUC scores of 0.75–0.85, meaning they correctly identify high-risk cases significantly better than random chance. In operational terms, this means early intervention resources can be directed at cases that genuinely need them rather than spread uniformly across all cases. No model is perfect, which is why human review of flagged cases remains essential.
NLP models trained specifically on occupational health documentation have demonstrated extraction accuracy rates of 90–95% for structured clinical fields in research settings. In production, accuracy depends heavily on the quality of the training data, the consistency of incoming document formats, and the implementation of human review workflows for edge cases. AI-extracted data should be treated as a first-pass structured summary for human review, not as a fully autonomous adjudication input.
What systems does AI occupational health software integrate with?
Mature occupational health AI platforms integrate with workers' compensation management systems, electronic health record (EHR) platforms, employer HRIS systems, and insurance claims platforms via HL7 FHIR, REST APIs, or direct database connectors. Integration depth varies significantly between vendors. Before selecting a platform, map your existing system landscape and confirm integration capability for each touchpoint in your RTW workflow.
How long does implementation typically take?
A focused implementation targeting a single workflow — automated intake and triage, for example — can go live in 8–12 weeks. A full-platform deployment covering intake, NLP processing, predictive analytics, automated communication, and case management integration typically takes 4–9 months depending on the complexity of the existing system landscape and the number of stakeholder groups requiring training and change management.
Last updated: September 2025